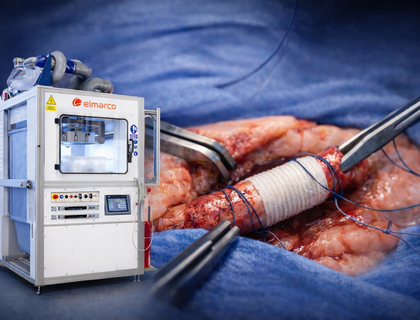
The potential of nanofibers in tissue engineering – carriers mimicking human tissue architecture!
Regenerative medicine is one of the most dynamically developing medical fields. Its main goal is to promote the recovery of diseased and damaged human tissue. The preparation of tissue and organ replacements depends on the structure of carriers (so‑called scaffolds) providing specific conditions for proper cell growth and the formation of whole tissue.
The architecture and the potential of these scaffolds have undergone great development in recent years. Scaffolds were made of metal, collagen, polyester foams, and hydrogel. But by far the best results are achieved with nanofibres, especially those created by the so‑called electrostatic spinning method.
What are the advantages of these nanofibres?
- They mimic the structure of the natural extracellular matrix in which cells are naturally held.
- They feature a small diameter that exactly matches the size of the extracellular matrix, making them ideal for attachment, proliferation for tissue renewal and cell differentiation, i.e. for the formation of functionally and structurally specialised cells.
- In addition, they can be designed to serve as transport means for bioactive factors, i.e. to transport growth factors and hormones in a controlled manner so that the “artificial tissue” grows properly.
- The scaffold components are bioactive (allowing controlled release of biomolecules according to the timeframe of tissue regeneration) and biodegradable (absorbed by the surrounding tissue without the need for surgical removal and without risk of damage to the new tissue).
Polymer nanofibres are used in many areas of tissue engineering because they are adaptable and structurally diverse. For example, for the aforementioned electrostatic spinning, classical, coaxial or alternating spinning methods can be used, as well as the Nanospider™ free surface spinning technology. The modification of the spinning nozzle allows the formation of fibres with unique structures and properties. The nanofibres can then feature any porosity, depending on the type of material, evaporation rate, and miscibility of the solvents used. This opens up the possibility of creating, for example, composite fibres for scaffolds that deliver the relevant biomolecules to the cells and have the ability to mechanically support the implanted cells even when the system fails.
Use of nanofibres in specific sub‑fields of tissue engineering
Although scientists are exploring the potential of nanofibres in various fields of tissue engineering, including growing whole organs, the most researched so far are musculature and bones. Regenerative medicine is most focused on promoting recovery of:
- Bone tissue,
- Skin,
- Musculature, and
- Cartilage.
 Interesting Fact: It is extremely difficult to grow an entire kidney or liver. These organs represent the highest level of complexity. In order to grow a kidney, scientists must first build a scaffold, fill it with stem cells, and use complex signalling to “invite” them to transform into blood vessel cells.
Interesting Fact: It is extremely difficult to grow an entire kidney or liver. These organs represent the highest level of complexity. In order to grow a kidney, scientists must first build a scaffold, fill it with stem cells, and use complex signalling to “invite” them to transform into blood vessel cells.
The potential of nanofibres in bone tissue architecture
The design of a carrier for bone tissue growth is based on the physical properties of bone, i.e. strength, porosity, hardness, and overall 3D structure. Mesenchymal stem cells (MSCs) are able to repair damaged tissue by transforming into a wide range of specialised cells, such as chondrocytes (cartilage cells), osteocytes (bone cells), neurons, and myocytes (muscle cells). This makes them the rarest candidates for use in regenerative medicine, as they can be grown in laboratories to produce almost any cell needed for tissue repair. Moreover, MCS grow beautifully on nanofibres, produce abundant extracellular matrix, and mineralise well.
 Tip: Composites based on collagen or gelatin nanofibres are most commonly used because they must have adequate porosity and morphology for transport of cells, nutrients, signalling molecules, gases, and metabolic products.
Tip: Composites based on collagen or gelatin nanofibres are most commonly used because they must have adequate porosity and morphology for transport of cells, nutrients, signalling molecules, gases, and metabolic products.
The potential of nanofibres in cartilage architecture
Cartilage tissue has a limited capacity for repair due to the reduced availability of chondrocytes. The chondrocyte is the basic cartilage cell, and its energy potential is unfortunately very limited. Most of its energy for protein production comes from anaerobic respiration because there is a lack of oxygen in the cartilage, i.e. it is not supplied with blood at all. The whole situation is complicated by the complete absence of progenitor cells in the vicinity of the injury. This is the baseline of cells, from which specialised chondrocytes would have developed. Cartilage does not contain blood vessels or nerves, and its nutrition is provided by intra‑articular fluid. However, this method of nutrition significantly limits the cartilage’s regenerative capacity – damage takes a long time to heal and, especially in the case of larger defects, cartilage does not fully recover. Therefore, one of the essential methods of cartilage tissue repair is the creation of a 3D nanofibrous carrier combined with chondrocytes and progenitor cells to ensure proper tissue growth and the formation of a complete connective tissue replacement.
 Tip: The goal of the cell carrier is to degrade after implantation in parallel with the formation of new healthy tissue, which over time will completely replace this nanofibrous 3D implant.
Tip: The goal of the cell carrier is to degrade after implantation in parallel with the formation of new healthy tissue, which over time will completely replace this nanofibrous 3D implant.
The potential of nanofibres in skin architecture
Skin wounds normally heal with scar tissue, i.e. connective tissue lacking elasticity. Scar tissue restricts tissue movement, often causes pain, and is aesthetically undesirable. The nanofibres of the carrier allow a “skin graft” to be grown and implanted on the wound, which then heals completely without scarring.
 Tip: Non woven silk fibroin is used, which is a nanofibre created by the well‑known electrospinning method. Due to its high porosity when coated with type I collagen, it has been found to best promote fibroblast adhesion and the growth of “new skin”.
Tip: Non woven silk fibroin is used, which is a nanofibre created by the well‑known electrospinning method. Due to its high porosity when coated with type I collagen, it has been found to best promote fibroblast adhesion and the growth of “new skin”.
Sources Cited:
- Liu, H., Ding, X., Zhou, G., Li, P., Wei, X., & Fan, Y. (2013). Electrospinning of nanofibers for tissue engineering applications. Journal of Nanomaterials.
- Vasita, R., & Katti, D. S. (2006). Nanofibers and their applications in tissue engineering. International Journal of nanomedicine, 1(1), 15.
- Nemati, S., Kim, S. J., Shin, Y. M., & Shin, H. (2019). Current progress in application of polymeric nanofibers to tissue engineering. Nano convergence, 6(1), 1‑16.
- Dahlin, R. L., Kasper, F. K., & Mikos, A. G. (2011). Polymeric nanofibers in tissue engineering. Tissue Engineering Part B: Reviews, 17(5), 349‑364.
- Ma, Z., Kotaki, M., Inai, R., & Ramakrishna, S. (2005). Potential of nanofiber matrix as tissue‑engineering scaffolds. Tissue engineering, 11(1‑2), 101‑109.
- Biomedical Nanotechnology. (2017). Nanotechnology in Tissue Engineering. P. Gopinath. YouTube video. [6.12.2021]. Available at: https://www.youtube.com/watch?v=4S1aqJnVaQE&t=1403s.